Home >> Complications, Doubts >> Frequent complications during pregnancy
Frequent complications during pregnancy
Loosening of the placenta
 Before the baby is born, the placenta can get loosened from the wall of the uterus as a result of a haemorrhage in the zone. The symptoms are strong pain in the abdomen together with an occasionally dark haemorrhage through the vagina.
Before the baby is born, the placenta can get loosened from the wall of the uterus as a result of a haemorrhage in the zone. The symptoms are strong pain in the abdomen together with an occasionally dark haemorrhage through the vagina.
It is associated to pre-eclampsia (arterial hypertension in some pregnant women) and usually happens in the third trimester. It can get to be serious, since the loosened part of placenta stops contributing oxygen to the baby, so once the problem is diagnosed, a caesarean section has to be made urgently.
Pre-eclampsia
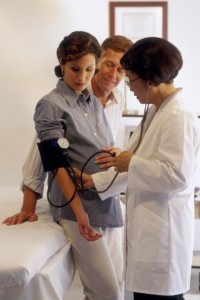
Pre-eclampsia is the arterial hypertension brought about by pregnancy. It occurs because the placenta creates some substances that contribute to obstruct arteries. Some signals of pre-eclampsia are: high blood pressure, swelling that does not disappear and an excessive amount of proteins in the urine.
To have high blood pressure does not necessarily mean to undergo pre-eclampsia. Your doctor will control it in each consultation and only when there is a worrisome decomposition could we speak of this disease.
It can bring about hypertensive crises to the mother, as well as hepatic or renal insufficiency, alterations of the coagulation and even convulsive or comatose reactions called eclampsia. In the baby it can produce a diminution of its growth or other complications like the placental loosening.
Placenta praevia
This is a complication in which the placenta is placed by itself in front of the head of the baby and covers the orifice in the neck of the uterus. This situation is frequent until week 20 of pregnancy. Nevertheless, if towards the date of the childbirth, the placenta continues to be located in this place, the vaginal childbirth becomes impossible and a caesarean section will be necessary. There can be some bleeding, which sometimes is normal. But if haemorrhage is abundant, this must be immediately treated.
Premature failure of the sac
The “breakage of the sac” consists of the loss of amniotic fluid through the genitals without being in labour. When the sac is broken, the germs in the neck of the uterus and the vagina can invade the amniotic fluid and can cause an infection to the baby. If you think that the sac has broken you must go immediately to a specialist. A vaginal examination will confirm or deny it. Often, the exit of liquid through the vagina is simply incontinence or abundant vaginal flow.
If the breakage takes place before week 32, your doctor will try to extend your pregnancy some weeks, because the premature risk is major that the one of fetal infection. The doctor will recommend you to rest, and will probably prescribe antibiotics and medication to accelerate the maturation of the baby’s lungs. In addition, the doctor will do a series of tests to you to diagnose infection signs. If the presence of infection is confirmed, they will bring about the child with the purpose of avoiding major risks for the baby. However this only happens in 2% of pregnancies.
Cutaneous eruptions
The most common cutaneous eruptions are gestational herpes and urticaria.
The term herpes is confused, because the problem is caused neither by a herpesvirus nor by other virus. It is thought that the cause of gestational herpes is some abnormal antibodies that react against tissues of your own body. This herpes is formed by blisters full of liquid and causes an intense itch.
As for urticaria, red, irregular, flat or slightly bulky spots appear, most frequently in the abdomen, which produce an intense itch in the abdomen. Sometimes they also have tiny blisters.
In order to deal with both types of cutaneous eruptions we have corticoids, which are applied with a cream or administered by oral route in the most serious cases.
Excessive vomiting (hyperemesis gravidarum)
The excess of vomiting during pregnancy, unlike habitual morning nauseas, is the extremely serious vomit presence that causes dehydration and starvation.
The cause of vomiting is not known, but psychological factors can influence much. Be careful because dehydration can bring about a haemorrhage in the retina of the eyes, dangerous alterations in the blood or injuries to the liver.
If your vomits are persistent, you must be hospitalized. Glucose or vitamin liquids will be administered to you via intravenous route. These will prevent you to eat and drink for at least 24 hours. If you need them, they will provide you drugs against nauseas and sedatives. Once the dehydration is surpassed, it is possible to begin eating little by little.
Viral respiratory infections (contagious)
These are contagious diseases that can affect the breathing and cause other symptoms. The most common symptoms in pregnancy are influenza, cold, chickenpox, infectious erythema, cytomegalovirus (CMV) and rubella (also called German measles).
 Anaemia
Anaemia
Anaemia is a diminution of the concentration of haemoglobin in the blood. The symptoms for the mother can be fatigue, lack of air and lack of energy. The baby will not be affected by this. The most common cause is the nourishing deficit. It is necessary to eat more. They will recommend you meals which are rich in iron, citruses juices and sometimes tablets with iron and folic acid. If the haemoglobin level descends alarmingly, a blood transfusion will be necessary.
Ectopic pregnancy
This happens when the fetus develops outside the uterus, whether it is in the Fallopian tube, the cervical channel or the pelvic or abdominal cavity. An ectopic pregnancy constitutes a risk for life and must be extirpated as soon as possible.
The symptoms of an ectopic pregnancy are small losses of blood by the vagina and abdominal pains like cramps.
Gestational diabetes
Hormones in the placenta can develop diabetes at the time of pregnancy. The treatment for gestational diabetes is a very strict diet as for carbohydrates. Not very often but insulin injections are necessary. A woman who has gone through diabetes in the gestation period must be put under a rigorous control. She has risks of suffering diabetes in coming years after childbirth or of having it again in future pregnancies.
Rh
Rh incompatibility is the incompatibility of the Rh group between the blood of the mother and the blood of her fetus. As a result, the woman can produce antibodies against red blood cells in the fetus. The antibodies cause the destruction of a more or less important number of these globules producing sometimes the denominated haemolytic disease of the new born, a variety of anaemia. In order to fight this anomaly there are different procedures that vary according to the seriousness. Antibodies anti-Rh in the Rh-negative mother can be injected. Sometimes, a transfusion of intrauterine blood is administered to the fetus. Only in some cases blood transfusions will be necessary to the baby when born.
Polyhydramnios and oligoamnios
We call polyhydramnios to the excess of amniotic fluid. Sometimes, this excess will be normal: when the baby is big or when the pregnancy is multiple. But this can also be a consequence of a disease of the mother like diabetes or a disease of the baby like the one called congenital malformations. Oligoamnios are the opposite, the diminution of the amount of amniotic fluid.
It is advisable to rest in order to avoid a premature childbirth. If there are respiratory difficulties, drainage off the excess of fluid by means of a puncture with an intra-amniotic catheter can be done.
Intrauterine growth retardation (IUGR)
We speak of retardation of the intrauterine growth when a baby is not growing within the uterus at the normal speed. At birth, these babies have usually a low weight and it is probable that they need to remain more time than normal in the hospital. Nevertheless, they reach a normal size around 2 years of age. Generally, these babies have a low weight when being born. Most of the cases of IUGR are out of the mother’s control. However, the consumption of tobacco, alcohol and other drugs can trigger this slowed down growth. You better leave these habits.
Multiple pregnancies
 A multiple pregnancy is a pregnancy considered to be of greater risk because it is associated to premature childbirth and development of pre-eclampsia. In addition, it is important to differentiate whether the babies are monozygotic or dizygotic twins. Monozygotic twins can share the placenta or sac, which can complicate the development during pregnancy and childbirth.
A multiple pregnancy is a pregnancy considered to be of greater risk because it is associated to premature childbirth and development of pre-eclampsia. In addition, it is important to differentiate whether the babies are monozygotic or dizygotic twins. Monozygotic twins can share the placenta or sac, which can complicate the development during pregnancy and childbirth.
Abortion
An (spontaneous) abortion is the loss of a fetus by natural causes before week 20 of pregnancy. However, the loss of a fetus by natural causes after week 20 of pregnancy is called dead fetus.
Before an abortion, the woman usually suffers little bleeding until she has a more evident haemorrhage together with vaginal secretion. The uterus contracts and the woman will feel a pain similar to cramps. If the abortion continues, the haemorrhage, the secretion and the pains increase. In the end, part or even all of the content of the uterus can be expelled. When only a part is expelled (incomplete abortion), an expansion and suction must be done to drain the uterus.
Tags: abortion, anaemia, anemia, baby, Complications, Cutaneous eruptions, diabetes, ectopic pregnancy, failure of the sac, gestation, IUGR, loosening of the placenta, mom, multiple pregnancy, placenta praevia, Polyhydramnios and oligoamnios, Pre-eclampsia, pregnancy, respiratory infections, rh, vomiting